Among equity and dignity – an article review by the NEXT Committee

An argument-based review of European ethical guidelines under COVID-19
This Article Review was prepared by Beatriz Lobo-Valbuena, Intensive Care Unit, Hospital Universitario del Henares, Madrid (Spain), on behalf of the NEXT Committee.
The COVID-19 pandemic has put national health systems against the ropes, requiring a reorganisation of the healthcare services whilst seeking a (complex) balance between public health ethics and patient-centred care. How can we establish a fair resource allocation and guarantee that the decisions are made ethically and consistently, rather than based on individual institutions or clinician’s approaches? Is there a way to find a balance between the principle of justice (equal distribution of resources and opportunities) and preserve patients’ autonomy? How can we solve the tension developed between the principles of utility (maximizing benefit) and equity (fair distribution of benefits and burdens), avoiding unwarranted variation of criteria that could threaten public health?
Perin and De Panfilis conducted an argument-based review of ethical guidelines to answer two questions:
- What are the ethical principles adopted by the ethical guidelines produced at the beginning of the COVID-19 outbreak related to resource allocation?
- What are the practical consequences of “priority” of access, access criteria, management of the decision-making process, and patient care?
After assessing 42 ethical guidelines through qualitative analysis (QUAGOL), 22 met inclusion criteria. Four ethical concepts and their related arguments were identified:
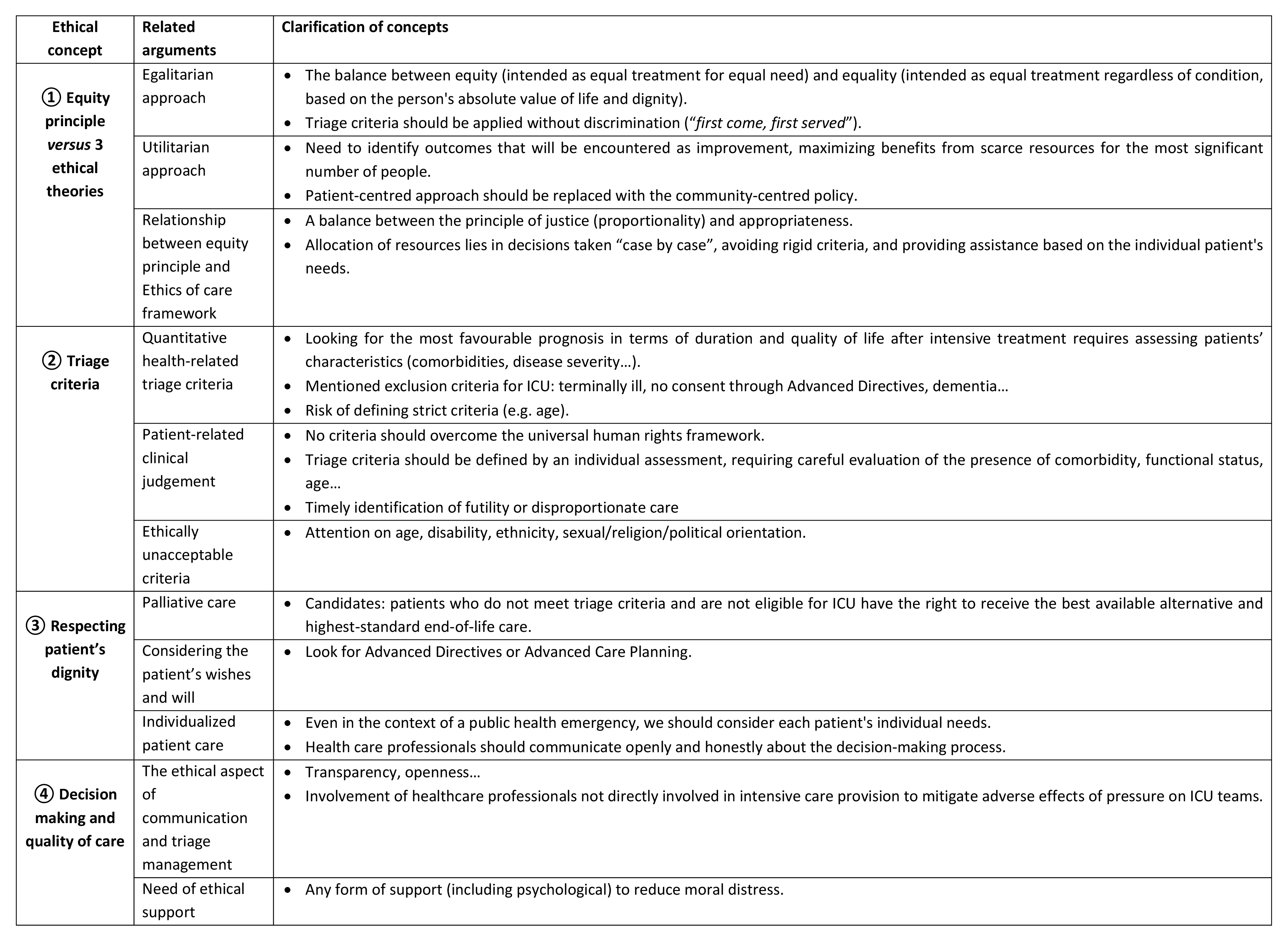
Each of the assessed guidelines recognized the respect for human life’s intrinsic value and the value of health as a human right, respecting patient’s choices, trying to reach a balance between appropriate and proportionate care, and deliberating about triage criteria in open and transparent communication.
This review also highlights the tension between respect for an equal right to health and the risk of taking triage decision, including potentially discriminatory criteria, with the risk of applying a severe utilitarian approach (considered in non-European guidelines). Moreover, even though we recognize the value of personalized care and the respect to patient’s values and opinions, “as scarcity increases, clinicians will increasingly be in a position in which they cannot respect all of the patient’s wishes, leading them to assume a paternalistic approach”.
TAKE-HOME MESSAGE
Current ethical guidelines try to figure out a way to personalize care, even in a pandemic situation. Allocating scarce resources should avoid unfair discrimination and consider patient’s choices and values. Therefore, personalized care should be developed by:

REFERENCE
Perin M. et De Panfilis L. ~ Among equity and dignity: an argument-based review of European ethical guidelines under COVID-19. BMC Med Ethics. 2021;22(1):36. doi: 10.1186/s12910-021-00603-9.
NEXT is a Steering Committee that speaks on behalf of trainees/young specialists and helps shape the future of the European Society of Intensive Care Medicine (ESICM) and of the discipline. Would you like to join us? Visit https://www.esicm.org/the-esicm/membership/ and follow us on Facebook | Twitter | Instagram.
Disclaimer: This short review was created because the original publication from which it is derived was judged to be relevant in the field of Intensive Care Medicine. The original publication is available for full consultation at the journal’s website. The creator is not related in any way to the original publication.